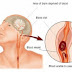
Vomiting is defined as the discharge of the contents of the stomach up into the mouth by force. Vomiting can be an attempt removing toxins from the gastrointestinal tract such as diarrhea, lower gastrointestinal tract.
Vomiting can be caused by many things such as the following:
Complications of vomiting are as follows :
Persistent vomiting can lead to complications of dehydration, electrolyte disturbances, rips Mallory Wiess, aspiration of gastric fluid.
Nursing Diagnosis for Vomiting
Risk for Fluid Volume Deficit related to the feeling of nausea and vomiting
Goal: Maintain the balance of fluid volume.
Outcomes: The client does not nausea and vomiting.
Intervention:
1. Monitor vital signs.
Rationale: An early indicator of hypovolemia.
2. Monitor intake and output and urine concentration.
Rationale: Decreased urine output and concentration will improve the sensitivity / sediment as one impression of dehydration and require increased fluids.
3. Give fluid little by little but often.
Rationale: To minimize the loss of fluids.
4. The risk of infection associated with an inadequate immune, characterized by: body temperature above normal. Increased respiratory rate.
Source : http://nurseskomar.blogspot.com/2013/10/nursing-diagnosis-for-vomiting-risk-for.html
Vomiting can be caused by many things such as the following:
- Congenital abnormalities
- Infection of the digestive tract
- Feeding the wrong way
- Poisoned
Complications of vomiting are as follows :
- Dehydration or alkalosis, due to loss of body fluid / electrolyte
- Ketosis from not eating and drinking
- Acidosis caused a sustained ketosis can be a shock even to seizures
- Abdominal muscle tension, conjunctival hemorrhage, esophageal rupture, aspirations, caused by severe vomiting.
Persistent vomiting can lead to complications of dehydration, electrolyte disturbances, rips Mallory Wiess, aspiration of gastric fluid.
Nursing Diagnosis for Vomiting
Risk for Fluid Volume Deficit related to the feeling of nausea and vomiting
Goal: Maintain the balance of fluid volume.
Outcomes: The client does not nausea and vomiting.
Intervention:
1. Monitor vital signs.
Rationale: An early indicator of hypovolemia.
2. Monitor intake and output and urine concentration.
Rationale: Decreased urine output and concentration will improve the sensitivity / sediment as one impression of dehydration and require increased fluids.
3. Give fluid little by little but often.
Rationale: To minimize the loss of fluids.
4. The risk of infection associated with an inadequate immune, characterized by: body temperature above normal. Increased respiratory rate.
Source : http://nurseskomar.blogspot.com/2013/10/nursing-diagnosis-for-vomiting-risk-for.html